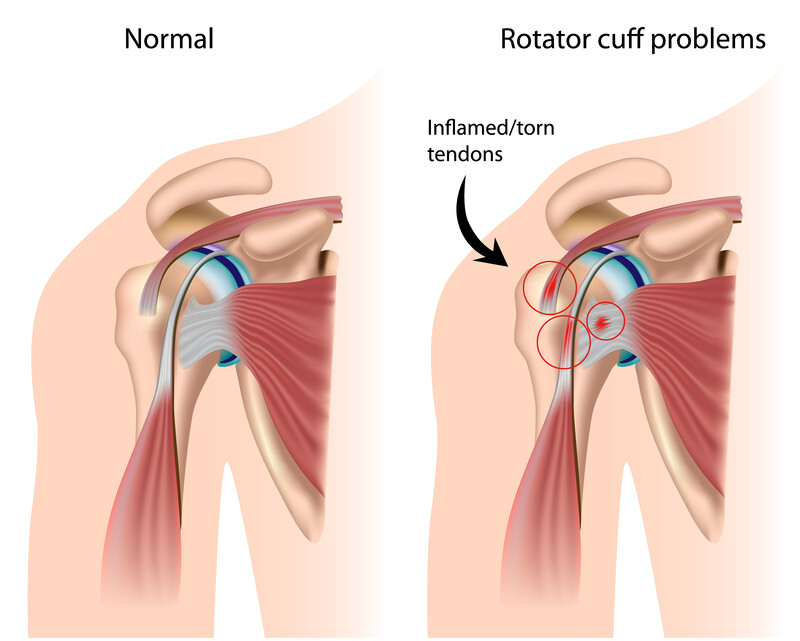
We often receive emails from people looking at their rotator cuff pain and tear treatment options. The emails we get center around the possible avoidance of rotator cuff surgery with regenerative medicine injection options. These options can include bone marrow aspirate injections or Platelet Rich Plasma therapy or PRP. There is some new research I will explore with you here on these rotator cuff treatment options. Hopefully this information will help you make an informed decision to have or not have these treatments.
We know that some people, like someone with a physically demanding job or an athlete, will make their decision as to how to treat their rotator cuff problems based on what treatment they believe will get them back to their job or sport the quickest. For some, rotator cuff surgery makes the most sense as the way to get them back quicker. These people, who believe that rotator cuff surgery is the fastest way back also have confidence that the surgery will make them whole again. For some people, rotator cuff surgery will get them back the quickest. For others not.
However, as pointed out in the research below, a great irony of rotator cuff surgery is that the patients believe it will work for them more than their surgeons will believe it will work for them.
If you went to an orthopedic surgeon, there is a good chance that he/she will follow the guidelines published in January 2022 in The Orthopedic clinics of North America journal. (1) Those guidelines are quoted here:
“Acute, traumatic rotator cuff tears typically occur in younger patients with a fall on an outstretched hand, grabbing an object to catch oneself when falling, or a glenohumeral dislocation. These tears are best evaluated with MRI. Partial-thickness tears may be managed nonoperatively with physical therapy, NSAIDs, and injections. Full-thickness tears in most patients should be managed with surgical repair as soon as possible, with better outcomes shown when repaired within 4 months of injury.”
Whether you chose to have surgery or not, it is apparent in many people that the rotator cuff tear should be dealt with in a timely fashion to prevent further shoulder deterioration.
A November 2021 study (2) points out that “Rotator cuff tear arthropathy (Rotator cuff tear degenerative disease) describes a pattern of glenohumeral degenerative changes following chronic rotator cuff tears that is characterized by superior humeral head migration (the ball of the shoulder is floating in the joint), erosion of the greater tuberosity (bone) of the humeral head, contouring of the coracoacromial arch to create a socket for the humeral head, and eventual glenohumeral arthritis. Acute and chronic inflammatory changes following rotator cuff tears are thought to contribute to cartilage damage, muscle fibrosis, and fatty infiltration in the glenohumeral joint.”
Many people have very good surgical results and they are satisfied with the outcomes. Many people have good success managing their shoulder pain with anti-inflammatory medications, physical therapy, the occasional cortisone injection and other non-surgical care methods. Nevertheless, we get many emails and phone calls from people wanting to know what their options are in regard to their shoulder problems. Some of these people are athletes or work at physically demanding lines of work and for them, surgery will be a down time that they would prefer to avoid.
Who do doctors suggest would be a good candidate for surgical treatment
A paper published in March 2020 (3) gives doctors a series of general recommendation of who should be sent to surgery and who should be recommended to non-surgical treatments.
In the try conservative non-surgical options first group are:
- People who have partial-thickness tears
- People who have large tears and the surgery to fix them may do more harm.
- People over the age of 65 years
- Degenerative full thickness tear but the patient’s shoulder is still stable
A July 2022 paper (4) suggested these clinical guidelines for helping workers with rotator cuff problems get back to work: “The initial assessment should include the patient’s history, a subjective assessment, and a physical examination. Diagnostic imaging is only necessary in select circumstances. Acetaminophen, non-steroidal anti-inflammatory drugs, and injection therapies may be useful to reduce pain in the short term. Clinicians should prescribe an active and task-oriented rehabilitation program (exercises and education) to reduce pain and disability in adults with rotator cuff disorders. Subacromial decompression is not recommended to treat rotator cuff tendinopathy. Surgery is appropriate for selected patients with a full-thickness rotator cuff tear. A return to work plan should be developed early . . .”
There is often disappointment when physical therapy or exercise does not work.
An August 2022 study (5) examines the routine prescribing of exercise for rotator cuff-related shoulder pain. The researches write: “Exercise is considered to be both essential and at the forefront of the management of rotator cuff-related shoulder pain. Despite this, many fail to substantially improve with exercise-based treatment. . . . The causal explanation for the beneficial effect of exercise for rotator cuff-related shoulder pain in clinical research is dominated by biomedical mechanisms (physical injury), despite a lack of supporting evidence.”
This disappointment in exercise’s failure can lead the patient to make a surgical decision.
Patient confidence in rotator cuff surgery is high. Research suggests that confidence may be unfounded and misguided.
“The results of (rotator cuff surgery) are not as predictable as the patient, family, trainer, coach and doctor would like to think.”
According to one athletic study from Loyola University Health System: “The results of (rotator cuff) treatment are not as predictable as the patient, family, trainer, coach and doctor would like to think.”(6) Further, these authors suggest: “Shoulder pain in the throwing athlete can present at any age and in any level of sport and can lead to dysfunction. A thorough evaluation of the throwing athlete can often determine the cause of symptoms, which is frequently multifactorial. Although the pathophysiology leading to pain in the shoulder of the throwing athlete is not entirely known, nonoperative modalities remain the mainstay of treatment. In general, surgical intervention should be reserved as a last resort. Effective treatment often requires collaboration among trainers, players, physicians, and therapists to determine an appropriate course of action.”
- Doctors at the University of Montreal suggest that “Despite improvements in rotator cuff surgery techniques, re-tear rate remains above 20% and increases with tear severity. Early rehabilitation exercises could contribute to re-tear due to excessive stresses.”(7)
There has long been a debate over the effectiveness of rotator cuff tear surgery. Numerous medical studies have shown that the re-tear rate of a surgically repaired shoulder could be anywhere from 20 – 90% depending on the patient circumstance. Australian researchers, presenting at the American Academy of Orthopaedic Surgeons (AAOS) 2012 Annual Meeting said that the failure rate they measured in 500 patients was 57%. In 2020, eight years later a March 2020 study (8) suggested: “patient-reported re-tear rate was 32.6%, and the reoperation rate was 34.7%”
- University Hospitals of Geneva on failed surgical repair: “Tear recurrence can be related to various factors such as:
- (1) inadequate strength of the initial rotator cuff repair construct,
- (2) biological failure to heal despite strong initial fixation (rotator cuff hardware and suture) and
- (3) inappropriate postoperative rotator cuff rehabilitation causing structural failure of the repair”(9)
Patients at greater risk for rotator cuff revision surgery if they have had a history of cortisone injections
An December 2019 (10) study in the journal Radiology described four main adverse findings that have been structurally observed in patients after cortisone injections.
- Cortisone injections accelerates the progression of degenerative arthritis.
- Cortisone injections weakens bone and causes fracture.
- Cortisone injections causes bone death and complications of osteonecrosis.
- Cortisone injections cause rapid joint destruction.
The problem of failed rotator cuff surgery
A study from the Mayo Clinic (11) discussed the problem younger people face who had a failed rotator cuff surgery. The study authors write: “Management of failed rotator cuff repair may be difficult, especially in young patients. Various non-modifiable and modifiable patient factors, including age, tendon quality, rotator cuff tear characteristics, acute or chronic rotator cuff tear, bone quality, tobacco use, and medications, affect rotator cuff repair healing. Surgical variables, such as the technique, timing, tension on the repair, the biomechanical construct, and fixation, as well as the postoperative rehabilitation strategy also affect rotator cuff repair healing.”
This research was noted in an October 2020 study (12) that assessed the use of cortisone in rotator cuff injury: “Multiple database studies have evaluated the relationship of steroid injections and rotator cuff repair outcomes and have found that steroid injections prior to rotator cuff repair have an increased risk of requiring revisions surgery compared with matched controls in a dose- and time-dependent manner.”
A December 2022 study (13) looked at patient outcomes following a revision rotator cuff repair. In this study 69 patients with an average age of 55 were followed after the second surgery to measure patient satisfaction. The initial findings showed the rotator cuff tendons did not heal to the tuberosity (where the muscle attaches to the bone) in 36% of the shoulders (25 of 69) following revision cuff surgery. Further, in 13 of the 69 patients, infection developed.Overall, 25% of patients had unsatisfactory clinical results and 22% were disappointed or dissatisfied.
In 2021 this research was followed up in a study (14) suggesting: “Re-tear following rotator cuff repair is common and has been reported to range from between 13 and 94% despite satisfactory clinical outcomes following rotator cuff surgery. Various risk factors have been associated with an increased tear rate, including patient factors, tear and shoulder morphology, repair technique, and rehabilitation regimes. Different modes of rotator cuff failure have been described. The management of re-tear in patients following rotator cuff repair is challenging and depends on the age, functional status and requirements of the patient, and re-tear size and residual tendon length.”
What is cortisone doing to the rotator cuff?
Another December 2019 study (15) in the journal Arthroscopy suggests that a steroid injection in the shoulder prior to rotator cuff surgery, puts you at a greater risk for post-surgical shoulder complications and possiboly the need for a secondary or revision shoulder surgery. Here is what the study says: “Several recent clinical trials have demonstrated that corticosteroid injections are correlated with increased risk of revision surgery after arthroscopic rotator cuff repair. . . Caution should be taken when deciding to inject a patient (with steroid), and this treatment should be withheld if an arthroscopic rotator cuff repair is to be performed within the following six months.”
“Two or more cortisone injections was associated with a substantially increased risk of subsequent revision rotator cuff surgery.”
A January 2019 study (16) in the journal Arthroscopy examined the effects of one or multiple corticosteroid injections a patient received for shoulder pain prior to having rotator cuff surgery. Here were these findings:
- “A single shoulder injection within a year prior to arthroscopic rotator cuff repair was not associated with any increased risk of revision surgery; however, the administration of 2 or more injections was associated with a substantially increased risk of subsequent revision rotator cuff surgery.”
An October 2020 study (17) compared one PRP injection to one corticosteroid injection for rotator cuff pain relief and improved function in patients with rotator cuff tendinopathy and partial thickness rotator cuff tears. After the one injection, patients were followed and results recorded at six weeks, three and twelve months post-injection. The researchers observed that patients with partial rotator cuff tears or tendinopathy experienced improvement in pain after both ultrasound-guided corticosteroid and PRP injections. However the patients who received PRP had superior improvement in rotator cuff pain and function at short-term follow up (3 months). One injection of PRP is not the way we offer the treatment.
Treating rotator cuff: Rotator cuff surgery alternatives and rotator cuff repair
In many articles on this site I discuss the growing interest medical researchers have in cellular communication. This interest is based on observations that stem cells, when introduced into a damaged joint, spontaneously change the joint environment from diseased to healing by signaling the native healing cells to get ready to rebuild.
A recent paper from a research team in Australia (18) confirms how this change of joint environment works.
- When introduced into a diseased joint, bone marrow stem cells display plasticity and multipotency (the ability to change/morph into other cell types and multiply). They also signal the native stem cells to join them.
- They also send signals to suppress inflammatory T–cell proliferation (inflammation) and provide an anti-inflammatory effect.
- Stem cells express various growth factors – an array of bioactive molecules that stimulate local tissue repair – These growth factors, and the direct cell to cell contact between MSCs and chondrocytes (the present remaining cartilage cells in the joint), have been observed to influence chondrogenic differentiation and cartilage matrix formation – in simple terms – stem cells regenerated cartilage.
An August 2017 (19) study published in the Journal of clinical imaging science found: Ultrasound guided platelet rich plasma injection for partial rotator cuff tears is an effective procedure that leads to significant decrease in pain, improvement in shoulder functions, much cost-effective and less problematic compared to a surgical treatment. “There is conclusive benefit for reducing pain and improving shoulder function in partial rotator cuff tears with ultrasound-guided PRP. . . This study succeeded in demonstrating that those patients receiving PRP injections have decreased pain, healing properties, and superior functional outcomes.”
Oral and injected corticosteroids cause non-traumatic rotator cuff tear or rupture
A group of German doctors published an August 2021 paper (20) with the purpose of examining the association between oral and injected corticosteroids and subsequent non-traumatic rotator cuff tear or rupture.
A total of 10,986 patients were included in each group (oral and injected corticosteroids). For both steroid treatments, the researchers found a significant association with non-traumatic rotator cuff tear or rupture, whereby oral corticosteroids had a stronger impact. For oral corticosteroids, this association was largely unaffected by differences in total doses or latencies between therapy end and index date. Within the group who received injected corticosteroids, shorter latencies and total doses of 20 mg or more led to higher odds of non-traumatic rotator cuff tear or rupture.
Conclusion: “Oral and injected non-traumatic rotator cuff tear or rupture in patients treated in orthopedic practices in Germany, while analgesics such as NSAIDs were not.”
Retears after rotator cuff repair (RCR) have been associated with poor clinical results.
A July 2022 paper (21) looked at surgical outcomes following rotator cuff repair surgery and revision rotator cuff repair surgery.
- During a 40-month period, 100 patients who underwent arthroscopic revision rotator cuff repair were evaluated preoperatively, at 6 months, and at 24 months using the Constant score (grading the surgical outcomes as unsatisfactory; fair; good; very good; and excellent), the Oxford Shoulder Score (the degree in measurement of pain and function), and the Subjective Shoulder Value (shoulder function measured and assessed as a percentage of a normal shoulder). Tendon integrity at 2 years was analyzed using magnetic resonance imaging. A total of 13 patients (13%) were lost to follow-up, and 14 patients (14%) had a symptomatic retear before the 24 months follow-up.
Results: All clinical scores improved significantly during the study period:
- Constant score: preoperative average 44/100 (100 being best).
- At 6 months 58/100.
- At 24 months 69/100. A 25% betterment in score after 2 years.
- Oxford Shoulder Score: preoperative average 27/48 (48 being the best score):
- At 6 months 36/48 :
- At 24 months 40/48. Almost a 30% betterment in score after 2 years.
- Subjective Shoulder Value (measured at 0% no shoulder function to 100% normal shoulder function) preoperative average 43%:
- At 6 months 66%:
- At 24 months 75%
A retear rate of 51.8% (43/83) and a surgical revision rate of 12.6% (11/87) were observed.
Conclusion: “Although arthroscopic revision rotator cuff repair improved shoulder function, retears were frequent but usually smaller. Patients with retears, however, did not necessarily have poorer shoulder function. Patient satisfaction at 2 years was lower when primary open rotator cuff repair was performed, when a subscapularis tear or osteoarthritis was present, and when the rotator cuff retear was located at the musculotendinous junction. Patients with traumatic retears showed better functional improvement after revision.
Now let’s look at the rotator cuff and the effects of cellular communication on repairing rotator cuff tears.
Doctors at various medical universities (22) combined to publish new research on the need for alternatives to rotator cuff surgery. Enhancing cellular communication may be the answer.
“Rotator cuff tears are one of the most common shoulder problems that usually require operative treatments. Therapeutic options used to repair ruptured tendons have consisted of suture, autografts, allografts (transplants), and synthetic prostheses.
Although surgical treatments have improved dramatically up to now, shoulder pathology is still challenging to orthopedic surgery primarily because these injuries often respond poorly to treatment and require prolonged rehabilitation.
Recent attention has focused on several biologic pathways which can augment function to tendon healing, consequently leading to the identification of growth factors involved in this process.”
Their attention were drawn to cytokines – small protein messengers instrumental in setting up signalling networks between healing factors. How do you stimulate cytokines? One way is to introduce stem cells into their network.
Stem cells create a non-surgical healing environment and this is why researchers from around the world are now pointing towards stem cell therapy as the future of rotator cuff repair and even to repair failed surgery damage. Here is new research to support that observation:
- Doctors from numerous teaching universities in Portugal (23) published these findings: A new treatment approach (stem cell therapy for rotator cuff) for decreasing the characteristic muscle degeneration associated with chronic rotator cuff tears. This strategy is particularly important for patients whose tendon healing after later surgical repair could be compromised by the progressing degenerative changes.
- From the University of Michigan: “Rotator cuff injuries are associated with atrophy and fat infiltration into the muscle, commonly referred to as “fatty degeneration.” As the poor function of chronically torn muscles may limit recovery after surgical repair, there is considerable interest in finding therapies to enhance muscle regeneration.” Those therapies include stem cells which can can improve muscle regeneration in other chronic injury states, and may be beneficial to enhance the treatment and recovery of patients with chronic rotator cuff tears.(24)
Bone Marrow aspirated stem cells injected into the shoulder
A February 2022 paper (25) wrote: “Stem cell treatment for rotator cuff tears is a promising development because they have been shown to result in an anti-inflammatory response, improved tendon regeneration, optimized collagen fiber arrangement, higher load-to-failure, and higher tensile strength.”
One shot a month apart is not really PRP treatment
I get a lot of emails. In some of the emails the writer will recount to me that they had PRP treatment for a rotator cuff tear and it did not work. There are a lot of times Platelet-rich plasma for a rotator cuff will not work. One way it will not work is if you get a single Platelet-rich plasma injection into the shoulder, more or less at random, and then one month later you get it again. That is the way many doctors offer Platelet-rich plasma treatment. That is not the way I do PRP therapy injections for the shoulder.
In the American Journal of Sports Medicine, July 2019, (26) a team of doctors in Switzerland tried the one injection, repeated a month later type of PRP treatment for a rotator cuff tear. More specifically for an Interstitial Supraspinatus Tear, the tendon of the Supraspinatus muscle of the rotator cuff. One of the rotator cuff muscles. It should be noted that in this study, ultrasound was used to guide the single injection to the damaged injury site.
The PRP injection was given to some of the study participants and some participants acting as a “control” group received a simple saline injection. So what happened? The PRP did not work any better than the saline solution. Why? When I see someone in our office with shoulder pain and shoulder instability, an examination will usually reveal that there are many things going on in the shoulder beyond a single or isolated tear of the Supraspinatus tendon (the tendon itself has only one tear), and that the shoulder itself is a degenerating joint.
In the Orthopaedic journal of sports medicine, (27) researchers noted that in Partial articular supraspinatus tendon avulsion (PASTA) tears are often seen in shoulders of throwing athletes who have recurrent anterior glenohumeral (shoulder) instability. In other words, there are many things going on at once, isolating out one injury in the shoulder will not solve a problem of total shoulder breakdown. In the shoulder rotator cuff injuries usually do not occur as an isolated tear. There is a lot going on in rotator cuff injuries.
Cortisone and PRP
A November 2019 study published in the Journal of back and musculoskeletal rehabilitation (28) compared cortisone injections (pain management) and PRP injections. The results of this comparative study found in “patients with rotator cuff lesions (tears), corticosteroid injection provides short-term relief for pain, function, and quality of life, while PRP injection works for long-term wellbeing.”
No consensus regarding treatment of partial thickness tears that fail conservative treatment
More recently a May 2021 study (29) examined the problem of “no consensus regarding treatment of partial thickness tears that fail conservative treatment.” The purpose then of this study was to assess the effectiveness and safety of two injections of PRP into the rotator cuff who have failed other conservative treatments with follow up two years after the PRP treatments. The conclusion of This study was “PRP injection is a safe and effective treatment for rotator cuff injury in patients who have failed conservative treatment of activity modification and physical therapy without deterioration of results two years after treatment. Better results are obtained with greater structural tendon damage than in shoulders with inflammation without structural damage.”
Two PRP injections into the same shoulder works better and lasts at least two years
A May 2021 study (30) suggests “PRP injection is a safe and effective treatment for rotator cuff injury in patients who have failed conservative treatment of activity modification and physical therapy without deterioration of results two years after treatment. Better results are obtained with greater structural tendon damage than in shoulders with inflammation without structural damage.” The study authors add: “The most important findings of this study are that dual rotator cuff PRP injection is safe and produces consistently beneficial results in patients with partial rotator cuff tears that have failed conservative treatment. The results continued to show benefits at two years after the initial injection. None of the treated patients presented with an increase in symptoms that would indicate progression of rotator cuff pathology from partial to full thickness tear. This is the first study to show sustained improvement out to two years post injection. It is the first to report dual injection of the rotator cuff. In our opinion, (our) study helps establish PRP injection as the preferred treatment for partial rotator cuff tears that fail activity modification and physical therapy.”
Comparing single platelet-rich plasma injection with hyaluronic acid injection for partial-thickness rotator cuff tears
A June 2022 (31) paper presented a prospective, nonrandomized, comparative study. The aim of the study was to compare the effects of ultrasound-guided single PRP injection with three doses of hyaluronic acid injection, combination of post-injection rehabilitation, for treating partial-thickness rotator cuff tears. The people of this study received either ultrasound-guided PRP injection and rehabilitation exercise, or ultrasound-guided subacromial hyaluronic acid injection and rehabilitation exercise. Shoulder Pain and Disability Index (SPADI), range of motion (ROM), pain visual analog scale (VAS), and Constant-Murley Shoulder Score (CMSS) were recorded before injection, and at 1 and 3 months after injection.
In the PRP group, pain and function scores significantly improved at 1-month and 3-month follow up; flexion and abduction range of motion significantly increased at 3-month follow up. In the hyaluronic acid injection group, pain and function scores also significantly improved in the first and third months; flexion and active abduction range of motion significantly increased in the third month. The PRP group revealed significantly better passive abduction range of motion at third month than the hyaluronic acid injection group.
Conclusion: “Ultrasound-guided single PRP injection exhibited comparable benefit to three doses of hyaluronic acid injection in patients with partial-thickness rotator cuff tears short-termly, with an extended effect regarding passive shoulder abduction range of motion and functionality.
“PRP does seem to play an effective role in significantly reducing the re-tear rate in acute rotator cuff tears”
A June 2022 paper (32) suggested: “PRP does seem to play an effective role in significantly reducing the retear rate in acute rotator cuff tears and in preventing full-blown large tears in chronic rotator cuff tendinopathies. Since the retear rates after an arthroscopic repair of rotator cuff tear continue to be quite high, biologic methods of managing rotator cuff pathologies like PRP are gaining traction since they are said to improve bone-tendon healing, thereby reducing the chances of rupture, tear, or retears.”
In an editorial in the journal Arthroscopy (33) Dr. Eric Hoffman offers this viewpoint: “Studies investigating the effect of PRP on shoulder rotator cuff healing, clinical outcomes, and retear rates suggest that PRP has no effect on outcome and healing but potentially reduces re-tear rates. However, study quality is compromised . . . Until there are reliable and valid data available, the use of PRP in rotator cuff repair is not strongly supported and is at the discretion of the treating surgeon. The current evidence shows the superiority of PRP over hyaluronic acid and corticosteroids, and there is promise that PRP could be a useful adjunct promoting rotator cuff healing following surgical repair.”
Do you have a question about your partial thickness rotator tear or full thickness tear rotator cuff issues for Dr. Darrow?
Over the years we have helped many people with rotator cuff tears. When someone comes into our institute it is usually after the “conservative treatments” have failed and that a surgery is being strongly recommended. What people want is a realistic plan to get them to a pain-free range of motion in a functioning shoulder. Many times we can get people to this goal, many times we come close to getting people to this goal with significant improvement to their quality of life. There are times when we can only help a little. There are times we cannot help at all. People we cannot help would be significantly advanced tears and cases of degenerative shoulder disease. Perhaps 10 to 20% of patients who seek regenerative medicine will not be good candidates. This is why I invite people to email me to discuss before they make an appointment for treating rotator cuff. You can do so as well by using the form below. Use the form below and tell me about your shoulder problems and I will get back to you and we can explore the realistic healing options that we may be able to offer you.
References
1 Patel M, Amini MH. Management of Acute Rotator Cuff Tears. The Orthopedic clinics of North America. 2022;53(1):69-76.
2 Nelson GB, McMellen CJ, Kolaczko JG, Millett PJ, Gillespie RJ, Su CA. Immunologic Contributions Following Rotator Cuff Injury and Development of Cuff Tear Arthropathy. JBJS reviews. 2021 Nov 1;9(11):e21.
3 Keener JD, Patterson BM, Orvets N, Chamberlain AM. Degenerative rotator cuff tears: refining surgical indications based on natural history data. JAAOS-Journal of the American Academy of Orthopaedic Surgeons. 2019 Mar 1;27(5):156-65.
4 Lafrance S, Charron M, Roy JS, Dyer JO, Frémont P, Dionne CE, MacDermid JC, Tousignant M, Rochette A, Doiron-Cadrin P, Lowry V. Diagnosing, Managing and Supporting Return to Work of Adults with Rotator Cuff Disorders: A Clinical Practice Guideline. Journal of Orthopaedic & Sports Physical Therapy. 2022 Jul 27(0):1-37.
5 Powell JK, Schram B, Lewis J, Hing W. “You have (rotator cuff related) shoulder pain, and to treat it, I recommend exercise.” A scoping review of the possible mechanisms underpinning exercise therapy. Musculoskelet Sci Pract. 2022 Aug 8;62:102646. doi: 10.1016/j.msksp.2022.102646. Epub ahead of print. PMID: 35964499.
6 Nickolas G. Garbis, Edward G. McFarland. Understanding and Evaluating Shoulder Pain in the Throwing Athlete. Physical Medicine and Rehabilitation Clinics of North America, 2014; 25 (4): 735 DOI:10.1016/j.pmr.2014.06.009
7 Haering D, Blache Y, Raison M, Begon M. Mechanical risk of rotator cuff repair failure during passive movements: A simulation-based study. Clin Biomech (Bristol, Avon). 2015 Dec;30(10):1181-8.
8 Hoffman TW, Maher A, Leigh WB, Brick MJ, Caughey MA, Young SW. Medium-term outcomes of a cohort of revision rotator cuff repairs. Journal of Shoulder and Elbow Surgery. 2020 Mar 4.
9 Lädermann A, Denard PJ, Burkhart SS. Management of failed rotator cuff repair: a systematic review. J ISAKOS. 2016 Jan;1(1):32-37. doi: 10.1136/jisakos-2015-000027. Epub 2016 Jan 21. PMID: 27134759; PMCID: PMC4849215.
10 Kompel AJ, Roemer FW, Murakami AM, Diaz LE, Crema MD, Guermazi A. Intra-articular corticosteroid injections in the hip and knee: perhaps not as safe as we thought?. Radiology. 2019 Dec;293(3):656-63.
11 Elhassan BT, Cox RM, Shukla DR, Lee J, Murthi AM, Tashjian RZ, Abboud JA. Management of failed rotator cuff repair in young patients. JAAOS-Journal of the American Academy of Orthopaedic Surgeons. 2017 Nov 1;25(11):e261-71.
12 Jensen AR, Taylor AJ, Sanchez-Sotelo J. Factors influencing the reparability and healing rates of rotator cuff tears. Current Reviews in Musculoskeletal Medicine. 2020 Jul 17:1-2.
13 Azar M, Van der Meijden O, Pireau N, Chelli M, Gonzalez JF, Boileau P. Arthroscopic Revision Cuff Repair: Do Tendons have a Second Chance to Heal?. Journal of Shoulder and Elbow Surgery. 2022 Jun 6.
14 Mandaleson A. Re-tears after rotator cuff repair: Current concepts review. Journal of Clinical Orthopaedics and Trauma. 2021 May 21.
15 Puzzitiello RN, Patel BH, Nwachukwu BU, Allen AA, Forsythe B, Salzler MJ. Adverse impact of corticosteroid injection on rotator cuff tendon health and repair: A systematic review. Arthroscopy: The Journal of Arthroscopic & Related Surgery. 2019 Dec 17.
16 Desai VS, Camp CL, Boddapati V, Dines JS, Brockmeier SF, Werner BC. Increasing numbers of shoulder corticosteroid injections within a year preoperatively may be associated with a higher rate of subsequent revision rotator cuff surgery. Arthroscopy: The Journal of Arthroscopic & Related Surgery. 2019 Jan 1;35(1):45-50.
17 Kwong CA, Woodmass JM, Gusnowski EM, Bois AJ, Leblanc J, More KD, Lo IKY. Platelet Rich Plasma in Patients with Partial Thickness Rotator Cuff Tears or Tendinopathy Leads to Significantly Improved Short-Term Pain Relief and Function Compared to Corticosteroid Injection: A Double-blind Randomized Controlled Trial. Arthroscopy. 2020 Oct 27:S0749-8063(20)30893-8. doi: 10.1016/j.arthro.2020.10.037.
18 Seol D, Zhou C, et al. Characteristics of meniscus progenitor cells migrated from injured meniscus. J Orthop Res. 2016 Nov 3. doi: 10.1002/jor.23472.
19 Sengodan VC, Kurian S, Ramasamy R. Treatment of Partial Rotator Cuff Tear with Ultrasound-guided Platelet-rich Plasma. J Clin Imaging Sci. 2017 Aug 14;7:32. doi: 10.4103/jcis.JCIS_26_17. PMID: 28900553; PMCID: PMC5582534.
20 Garthe TL, Jacob L, Kostev K. Association between corticosteroid therapy and diagnosis of non-traumatic rotator cuff tear or rupture in patients followed in orthopedic practices in Germany. International Journal of Clinical Pharmacology and Therapeutics. 2021 Aug 23.
21 Hackl M, Flury M, Kolling C, Nebelung W, Krauss CA, Kraemer NA, Heuberer PR, Laky B, Wellmann M, Pastor MF, Imhoff AB. Results of Arthroscopic Revision Rotator Cuff Repair for Failed Open or Arthroscopic Repair: A Prospective Multicenter Study on 100 Cases. The American Journal of Sports Medicine. 2022 Jun 6:03635465221097410.
22 Wu G et al. Advances in the treatment of rotator cuff lesions by cytokines. Front Biosci (Landmark Ed). 2017 Jan 1;22:516-529.
23 Sevivas N, Teixeira FG, Portugal R, Araújo L, Carriço LF, Ferreira N, Vieira da Silva M, Espregueira-Mendes J, Anjo S, Manadas B, Sousa N, Salgado AJ. Mesenchymal Stem Cell Secretome: A Potential Tool for the Prevention of Muscle Degenerative Changes Associated With Chronic Rotator Cuff Tears. Am J Sports Med. 2016 Aug 8. pii: 0363546516657827.
24 Gumucio JP, Flood MD, Roche SM, Sugg KB, Momoh AO, Kosnik PE, Bedi A, Mendias CL. Stromal vascular stem cell treatment decreases muscle fibrosis following chronic rotator cuff tear. Int Orthop. 2016 Apr;40(4):759-64. doi: 10.1007/s00264-015-2937-x.
25 Thangarajah T, Lo IK. Optimal Management of Partial Thickness Rotator Cuff Tears: Clinical Considerations and Practical Management. Orthopedic Research and Reviews. 2022;14:59.
26 Schwitzguebel AJ, Kolo FC, Tirefort J, Kourhani A, Nowak A, Gremeaux V, Saffarini M, Lädermann A. Efficacy of platelet-rich plasma for the treatment of interstitial supraspinatus lesions: A randomized, double-blinded, controlled trial: PRP for Interstitial Supraspinatus Lesions. Orthopaedic Journal of Sports Medicine. 2019 May 31;7(5_suppl3):2325967119S00210.
27 Ueda Y, Sugaya H, Takahashi N, Matsuki K, Tokai M, Hoshika S, Onishi K, Hamada H. Prevalence and Site of Rotator Cuff Lesions in Shoulders With Recurrent Anterior Instability in a Young Population. Orthop J Sports Med. 2019 Jun 4;7(6):2325967119849876. doi: 10.1177/2325967119849876. PubMed PMID: 31211152; PubMed Central PMCID: PMC6552367.
28 Sari A, Eroglu A. Comparison of ultrasound-guided platelet rich plasma, prolotherapy, and corticosteroid injections in rotator cuff lesions. Journal of back and musculoskeletal rehabilitation. 2019 Nov 8(Preprint):1-0.
29 Prodromos CC, Finkle S, Prodromos A, Chen JL, Schwartz A, Wathen L. Treatment of Rotator Cuff Tears with platelet rich plasma: a prospective study with 2 year follow‐up. BMC Musculoskeletal Disorders. 2021 Dec;22(1):1-3.
30 Prodromos CC, Finkle S, Prodromos A, Chen JL, Schwartz A, Wathen L. Treatment of Rotator Cuff Tears with platelet rich plasma: a prospective study with 2 year follow‐up. BMC Musculoskeletal Disorders. 2021 Dec;22(1):1-3.
31 Huang SH, Hsu PC, Wang KA, Chou CL, Wang JC. Comparison of single platelet-rich plasma injection with hyaluronic acid injection for partial-thickness rotator cuff tears. Journal of the Chinese Medical Association. 2022 Jun 1;85(6):723-9.
32 Bhan K, Singh B. Efficacy of Platelet-Rich Plasma Injection in the Management of Rotator Cuff Tendinopathy: A Review of the Current Literature. Cureus. 2022 Jun 20;14(6).
33 Hohmann E. Editorial Commentary: Platelet-Rich Plasma Reduces Retear Rates Following Rotator Cuff Repair but Does Not Improve Clinical Outcomes. Arthroscopy: The Journal of Arthroscopic & Related Surgery. 2022 Aug 1;38(8):2389-90.